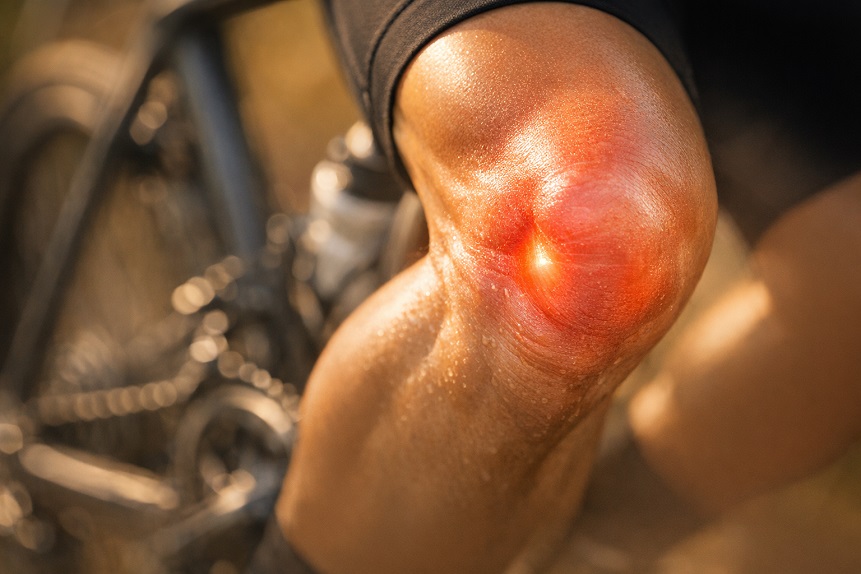
Cycling frequently appears on lists of recommended activities for people with joint problems, and the recommendation is not wrong. Compared to running, cycling removes the impact loading that places high peak forces on the lower extremity joints, making it a genuinely more comfortable option for people whose joints struggle with impact. But “lower impact than running” is not the same as “without joint stress,” and cyclists who log significant hours in the saddle know from experience that the bike has its own specific pattern of joint demands that can produce discomfort just as reliably as impact sports, through entirely different mechanisms.
The combination of a fixed pedalling motion repeated thousands of times per ride, a riding position that constrains joints within narrow ranges for extended periods, and the power demands of climbing and interval training creates a joint stress profile that is quite specific to cycling. Understanding it is the first step to managing it, and the cyclists who ride most comfortably for decades are the ones who understand where their vulnerable points are before those points start announcing themselves.
Here is the cycling-specific joint picture, joint by joint, and what a practical joint health strategy for cyclists looks like.
Contents
The Knee: Cycling’s Most Commonly Affected Joint
Knee pain is the most prevalent joint complaint among cyclists, and the reasons are well-established in sports medicine. A recreational cyclist completing a two-hour ride at 80 rpm is performing approximately 9,600 pedal strokes. Each stroke involves the knee cycling through a specific arc of flexion and extension, and the joint structures engaged depend on where in the pedal stroke the greatest force is being applied. The patellofemoral joint, where the kneecap tracks across the femoral groove during knee flexion and extension, is particularly susceptible to cycling-related stress because it is loaded repeatedly through the mid-range of knee flexion where patellofemoral contact force is highest.
Bike Fit: The Variable That Determines Almost Everything
More than almost any other sport, cycling allows the mechanical environment of the joint to be adjusted externally through bike fit. Saddle height is the single most important fit variable for knee health: a saddle too low creates excessive knee flexion at the bottom of the pedal stroke, increasing compressive patellofemoral forces and the risk of medial knee pain; a saddle too high causes the hip to rock at the top of the stroke, creating lateral tracking issues and Iliotibial Band (ITB) tension that loads the lateral knee compartment. Saddle fore-aft position affects the angle at which the quadriceps apply force through the patella, directly influencing patellofemoral joint stress distribution. Cleat position and float determine the degree of rotational freedom available at the ankle, which affects alignment through the entire lower extremity kinetic chain including the knee. A professional bike fit is the most impactful single investment a serious cyclist can make in their joint health. Glucosamine Sulfate 2KCL and Phytodroitin™ support the patellofemoral and tibiofemoral cartilage that bears the repetitive loading of pedalling, providing the structural maintenance support that the high-turnover demands of regular cycling create.
The ITB and Lateral Knee
The iliotibial band, a thick fibrous structure running from the hip down the outside of the thigh to attach below the knee, is not a joint structure but its tension directly affects lateral knee and hip joint mechanics in cyclists. ITB syndrome, characterised by sharp lateral knee pain on the downstroke, is one of the most common overuse injuries in cyclists and reflects the interaction between saddle height, cleat position, and hip abductor strength imbalances. The anti-inflammatory support of CurcuWIN® and AprèsFlex® is relevant to the local inflammatory response that drives the pain of ITB syndrome, and the collagen synthesis support of OptiMSM® is relevant to the structural maintenance of the band itself.
The Hip: Where the Pedalling Engine Originates
The hip generates the primary power of the pedal stroke through the gluteal and hamstring muscles, and the hip joint itself experiences the reaction forces of this power generation across thousands of repetitions per ride. In the aerodynamic positions favoured by road cyclists, the hip is maintained in a degree of flexion that restricts its range of motion and loads the anterior hip capsule in a manner similar to, though less extreme than, prolonged sitting. This anterior hip compression combined with the repetitive hip flexion-extension of pedalling creates a specific loading pattern on the hip cartilage and labrum that differs from the hip stress of running or strength training but is no less real in its cumulative potential.
Hip flexibility limitations, particularly restricted hip flexor length and reduced internal rotation, compound this stress by altering pedalling mechanics and forcing compensations into the lumbar spine and knee. Cyclists who notice hip tightness, groin discomfort at the end of long rides, or reduced hip range of motion compared to their non-cycling peers are observing a pattern that responds well to hip mobility work, saddle height optimisation, and the anti-inflammatory support that addresses the low-grade synovial inflammation in the hip joint that typically precedes more significant symptoms. For context on the connection between joint inflammation and cartilage health, our article on the difference between joint pain and inflammation is useful background.
The Ankle and Foot: The Often-Forgotten Foundation
The ankle is the transmission point between the leg’s power output and the pedal, and it operates within the constraints of cleat position, shoe stiffness, and individual foot biomechanics. Most cyclists use stiff-soled shoes specifically to minimise energy loss at the ankle, which is efficient but means the ankle joint itself is not performing the dynamic flexion-extension movement it would in running or walking. Instead, it holds a relatively fixed position through the pedal stroke while experiencing the transmission of significant pedalling forces.
The subtalar joint, responsible for the inward and outward rolling of the foot, is particularly relevant to cyclists because foot pronation or supination in the shoe directly affects knee and hip alignment through the kinetic chain. Cleats that are positioned too far inward or outward relative to the natural foot angle create rotational stress at the ankle and knee through the entire pedal stroke. Ankle and foot joint problems in cyclists are often traced to cleat position and are frequently amenable to fit adjustments, but the cumulative loading they represent warrants nutritional support for the articular cartilage and connective tissue of the ankle as much as the knee and hip.
A Joint Health Strategy for Consistent Cyclists
The cycling-specific joint health strategy that serves riders best over years and decades combines three elements: bike fit optimisation that distributes joint loading appropriately, off-bike mobility and strength work that maintains the range of motion and muscular balance that cycling position gradually reduces, and nutritional support that addresses the connective tissue demands of high-volume repetitive pedalling.
On the nutritional side, the combination of structural cartilage support from Glucosamine Sulfate 2KCL and Phytodroitin™, collagen synthesis and tendon support from OptiMSM®, and multi-pathway anti-inflammatory management from CurcuWIN® and AprèsFlex® addresses the complete joint health picture for cyclists. The volume demands of cycling, particularly for riders logging six or more hours per week, place meaningful ongoing demands on cartilage matrix turnover that nutritional support can meaningfully help the body meet. The inflammatory component is equally important: high-volume training generates an inflammatory burden that, managed effectively through anti-inflammatory nutrition, does not accumulate into the chronic joint inflammation that impairs both comfort and training capacity.
For cyclists who also want to understand the broader lifestyle and nutritional framework within which joint supplementation sits, our guide to building a complete joint health routine covers the full picture beyond supplementation alone.
Frequently Asked Questions
- Is cycling recommended for people who already have knee arthritis?
- Cycling is generally considered one of the most appropriate aerobic activities for people with knee osteoarthritis specifically because it removes the impact loading that exacerbates cartilage stress. The low-impact repetitive motion maintains joint mobility, muscle strength around the knee, and cardiovascular fitness without the peak force spikes of walking on hard surfaces or any impact sport. Resistance should be kept comfortable and saddle height carefully optimised to minimise compressive patellofemoral forces. Many rheumatologists and physiotherapists specifically recommend cycling as a primary exercise modality for knee osteoarthritis management.
- Should cyclists take joint supplements year-round or only during high-volume training periods?
- Year-round supplementation is more consistent with the biology of how structural joint support ingredients work. Glucosamine and MSM operate through slow-building mechanisms that maintain tissue quality over time rather than spiking and declining with training load. Stopping supplementation during off-season or lower volume periods removes the ongoing maintenance support that keeps cartilage matrix quality stable. The anti-inflammatory ingredients are relevant during periods of higher training load but do no harm during lower-volume periods. Consistent year-round use is the most rational approach for any cyclist who trains regularly across the year.
- Can joint supplements help with saddle-related discomfort?
- Saddle discomfort in cyclists primarily involves soft tissue compression of the perineal area and ischial tuberosities rather than joint-specific issues, and is primarily addressed through saddle choice, position, and cycling shorts quality rather than joint supplementation. Where saddle issues have contributed to hip or lower back compensations that create secondary joint stress, anti-inflammatory support from CurcuWIN® and AprèsFlex® may help manage that secondary inflammatory response. But the primary intervention for saddle-related discomfort is fit and equipment, not nutrition.
- Is cycling indoors on a trainer better or worse for joints than outdoor cycling?
- Indoor training on a fixed trainer eliminates the lateral weight shifts, varied terrain responses, and small positional adjustments that outdoor cycling naturally includes. This can make indoor training marginally more repetitive in terms of joint loading patterns, since the bike is fixed and the rider does not make the micro-adjustments that outdoor riding demands. For extended indoor training blocks, incorporating deliberate positional variation, including out-of-the-saddle intervals and varied cadence work, reintroduces some of the movement variety that static indoor riding lacks. The difference is modest and should not deter anyone from indoor training for practical reasons.
Cycling is a wonderful sport for joint health at the right doses, with the right fit, and with the right support in place. The riders who experience the most joint difficulties are rarely those who cycle too much in any absolute sense: they are most often those who cycle in a position that concentrates stress inappropriately, without the off-bike work that maintains the mobility cycling progressively reduces, and without the nutritional support that high-volume cartilage and tendon loading demands. Getting those three dimensions right makes decades of comfortable riding an entirely realistic goal.