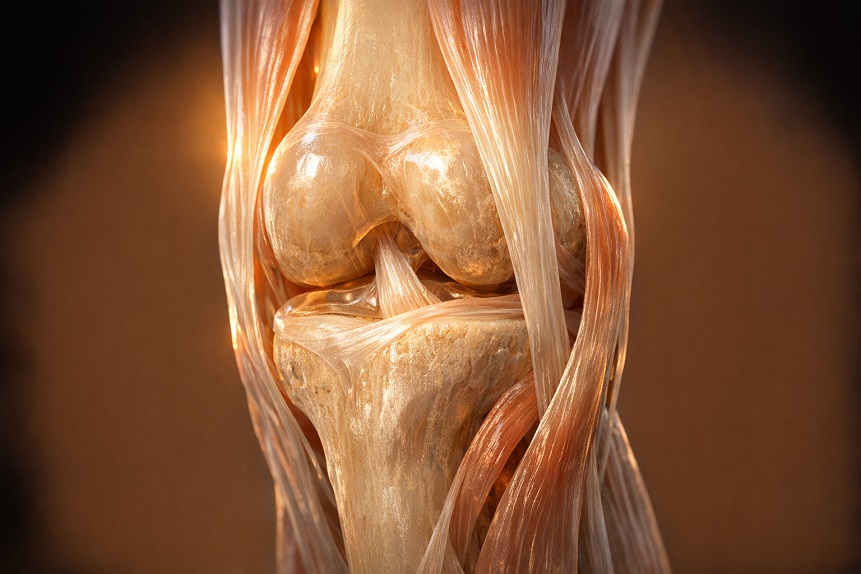
Picture a door hinge. A well-oiled one swings open silently, effortlessly, year after year. A neglected one squeaks, stiffens, and eventually seizes up entirely. Your joints operate on a surprisingly similar principle, except that instead of metal and oil, the engineering relies on a remarkable combination of living tissues, each one with a specific job to do.
Most people give their joints very little thought until something goes wrong. Then suddenly they are very interested in what exactly is happening in there. That curiosity is worth following, because understanding your joint anatomy is genuinely the most useful starting point for anyone who wants to protect their mobility or address discomfort that has crept in over time.
This article walks through the main structural components of a joint, what each one contributes to healthy movement, and what happens when any part of the system starts to struggle. No medical degree required.
Contents
- The Architecture of a Synovial Joint: More Complex Than You Might Expect
- Synovial Fluid: The Lubricant That Also Feeds Your Cartilage
- Tendons and Ligaments: The Cables That Hold Everything Together
- How All These Components Work as a System (And Why That Matters for How You Support Them)
- Frequently Asked Questions
The Architecture of a Synovial Joint: More Complex Than You Might Expect
The joints that give us the widest range of motion, including knees, hips, shoulders, and knuckles, are called synovial joints. They are the ones most relevant to the kind of stiffness and discomfort that brings people to a site like this one. A synovial joint is not simply two bones touching. It is a carefully designed system with several interdependent components, and the health of each one affects all the others.
Cartilage: The Shock Absorber That Cannot Heal Itself
Articular cartilage is the smooth, pearlescent tissue that covers the ends of bones where they meet inside a joint. Run your thumb across the end of a chicken drumstick and you will feel it: firm, glassy, slightly springy. That is cartilage. In a healthy joint it allows bones to glide across one another with almost no friction. The problem is that cartilage has very limited blood supply, which means it gets its nutrients through a process of compression and release rather than direct circulation. This also means that when cartilage is damaged, it heals poorly or not at all. Think of it as the one component in the system that you genuinely cannot afford to neglect, because replacing it is not straightforward. Compounds like Glucosamine Sulfate 2KCL and Phytodroitin have attracted significant research interest precisely because of their role in supporting the structural integrity of cartilage tissue.
Subchondral Bone: The Foundation Beneath the Cushion
Directly beneath cartilage lies subchondral bone, a dense layer that acts as a secondary shock absorber. Healthy subchondral bone is firm but slightly elastic, helping to distribute the forces transmitted through a joint during impact activities like running or jumping. When cartilage thins with age or overuse, subchondral bone is often the first place changes show up on an imaging scan. The two tissues are more interconnected than they might appear, and researchers now understand that you cannot fully consider the health of one without the other.
Synovial Fluid: The Lubricant That Also Feeds Your Cartilage
Inside every synovial joint is a sealed cavity containing synovial fluid, a viscous, egg-white-like substance produced by the synovial membrane that lines the joint capsule. This fluid does two jobs simultaneously. First, it lubricates the joint, reducing friction between cartilage surfaces during movement. Second, and this is the part that often surprises people, it delivers oxygen and nutrients to the cartilage. Because cartilage has no direct blood supply, it relies almost entirely on synovial fluid for its nourishment. This is one of the reasons why gentle, regular movement tends to support joint health better than extended periods of stillness: movement pumps fresh synovial fluid into contact with cartilage, while inactivity starves it.
Synovial fluid also contains hyaluronic acid, a molecule that gives the fluid its characteristic thickness. As people age, synovial fluid can become thinner and less effective. This is part of why joints that felt fine at 35 can begin to feel grittier or less comfortable at 55, even without any significant cartilage damage having occurred. If you have ever noticed that your joints feel stiffer first thing in the morning but loosen up after ten minutes of movement, you have experienced this fluid dynamics principle in action. For a closer look at this particular phenomenon, our article on why joints get stiff with age unpacks the biology in detail.
Tendons and Ligaments: The Cables That Hold Everything Together
Joints would be entirely unstable without the connective tissues that anchor and guide them. Tendons and ligaments are both made primarily from collagen, but they serve very different functions and are often confused with each other.
Ligaments: Bone to Bone Stability
Ligaments connect bone to bone. Their job is to limit excessive joint movement and prevent dislocation. The ACL in your knee, for example, is a ligament. It is tight, slightly elastic, and built to resist the forces that would otherwise send your lower leg sliding forward relative to your upper leg during dynamic movement. Ligaments have a modest blood supply, which means they can heal from injury, but slowly and imperfectly. A significant ligament sprain often leaves behind slightly lax connective tissue, which is why previous joint injuries can increase long-term instability and discomfort. OptiMSM, a highly purified form of methylsulfonylmethane, is a compound that contributes sulfur to the body’s collagen synthesis process, making it relevant to the ongoing maintenance of connective tissue like ligaments.
Tendons: Muscle to Bone Power Transfer
Tendons connect muscle to bone. When your quadriceps contract to straighten your knee, it is the patellar tendon that transmits that force across the joint. Tendons are built for strength rather than flexibility. They are dense, fibrous, and remarkably tough under normal loading conditions. However, repetitive strain, particularly the kind that builds up gradually in athletes, manual workers, or people who perform the same movement thousands of times a day, can cause tendon tissue to degrade faster than it regenerates. This is a category of joint-adjacent damage that does not always show up as classic “joint pain” but is very much part of the broader picture of joint health over a lifetime.
How All These Components Work as a System (And Why That Matters for How You Support Them)
The practical takeaway from all of this anatomy is that joint health is not a single issue with a single solution. Cartilage, synovial fluid, subchondral bone, ligaments, and tendons each have distinct biological needs, different vulnerabilities, and different responses to the choices you make about movement, nutrition, and supplementation. Supporting cartilage structure requires different nutritional inputs than maintaining collagen-rich tendons and ligaments, for example, and neither of those is the same as preserving the quality and volume of synovial fluid.
This is why the most thoughtfully formulated joint supplements address multiple components of the system rather than focusing on a single ingredient. It is also why lifestyle factors, including how much you move, what you eat, and how well you sleep, have such a measurable effect on how your joints feel over time. The components described here do not operate in isolation. They are in constant conversation with each other, and with the rest of your body.
If you want to understand what happens when these components begin to change with age, Why Do Joints Get Stiff and Achy as You Age? is a natural next step. And if you are curious about how specific nutrients support cartilage at a structural level, our deep dive on Glucosamine Sulfate 2KCL covers the science in plain language.
Frequently Asked Questions
- Is cartilage the same thing as bone?
- No. Cartilage and bone are distinct tissues with different compositions and properties. Bone is mineralized and hard, with a good blood supply that allows it to repair after fracture. Cartilage is softer, flexible, and has very limited blood supply, which is why it heals poorly when damaged. In joints, cartilage covers bone ends to allow smooth, low-friction movement.
- Can you rebuild cartilage once it has worn down?
- Cartilage has very limited regenerative capacity because it lacks direct blood supply. Significant cartilage loss cannot currently be fully reversed through diet or supplementation alone. However, research suggests that certain compounds, including glucosamine and specific botanical extracts, may help slow further degradation and support the structural environment cartilage needs to function. Prevention and early support matter far more than late intervention.
- What is the difference between a tendon injury and a ligament injury?
- Tendons connect muscle to bone and are typically injured through overuse or sudden overload during activity. Ligaments connect bone to bone and are more commonly sprained through impact or excessive twisting forces. Both are collagen-rich tissues that heal slowly. Tendon injuries often present as gradual, activity-related pain; ligament injuries more often involve a specific incident followed by instability and swelling.
- Why do joints crack or pop during movement?
- Joint popping during movement is usually caused by one of two things: gas bubbles forming and collapsing in synovial fluid (the classic “knuckle crack”), or tendons and ligaments briefly snapping over bony prominences as the joint moves. Neither cause is inherently harmful in the absence of pain. Persistent clicking accompanied by discomfort or swelling, however, is worth discussing with a healthcare professional.
Understanding what your joints are made of is one of those pieces of knowledge that quietly changes how you think about everything else, from why a particular supplement ingredient makes sense to why certain exercises protect joints rather than stress them. When you are ready to go further, our guide to exercises that support joint health is a practical place to take what you have learned here and put it to work.